NURS FPX 9010 Assessment 2 Project Proposal
Student Name
Capella University
NURS-FPX9010 Doctor Of Nursing Practice 2
Professor Name
Submission Date
Project Proposal
In outpatient care, infusion-related issues have remained a problem as far as patient safety is concerned. In the current project site, a privately owned outpatient wellness and infusion center, baseline data illustrate that as much as 14 percent of infusion encounters had complications with being documented (Clinical Director, personal communication, January 15, 2026). Among the major causative factors, there were uneven IV site evaluation, the difference in following the aseptic technique, and procedures not being properly documented (Nickel et al., 2024). IV peripheral complications (i.e., phlebitis, infiltration, catheter occlusion) are something that brings discomfort to patients and introduces a break in the continuity of treatment (Marsh et al., 2024). Evidence-based best practices of care will be standardized, which will help address the gaps in patient safety and quality of care.
In nursing staff nurses (P) in the care of adults (C) receiving outpatient infusion therapy, the effect of the intervention with Infusion Nurses Society infusion therapy standards (including the use of structured IV site assessment and aseptic technique training, I) versus the current practice (C) on the occurrence of infusion-related complications (O) in eight weeks (T)? The published literature resulted in supporting a structured, comprehensive infusion care protocol that has been demonstrated to minimize peripheral IV catheters and enhance the accuracy of written documentation regarding the care of the catheters (Demiroglu and Tosun, 2025). The use of competency-based training to offer evidence-based principles to assess nursing practice in terms of the implementation of peripheral IV catheters enhances the level of compliance of nurses with standard assessment and infection prevention guidelines (Lewis et al., 2022). Evidence-based quality improvement initiatives have repeatedly shown that quantifiable reductions in preventable adverse patient events relating to infusion-related procedures in an ambulatory care setting are possible.
Practice Problem
Eight weeks of infusion record reviews revealed that out of every 14 infusion encounters, 14% of the encounters were linked with a complication over the eight weeks (Clinical Director, personal communication, January 15, 2026). Once again, phlebitis was the most prevalent complication at 6%, with infiltration (6%), and reinsertion of the catheter being necessary because of occlusion (3%). Repeat of these problems related to complications with medicine administration equipment and the absence of appropriate follow-up with the patients was an ongoing problem in the outpatient parenteral antimicrobial therapy programs on a global scale (Wolie et al., 2024). The evidence gathered by it has led to a huge disparity in the quality of service currently given to the patients at the place, which needs to be addressed urgently, according to the best scientific evidence available.
Absence of uniform clinical process and standardization in outpatient practices has been identified as one of the leading factors to preventable complications. The high patient-to-nurse ratios, inadequate interdisciplinary communication, and frequent changes in nursing personnel in the prospective study by Beaudart et al. (2023) created a significant number of medication errors associated with outpatient infusion therapy. The same issues regarding variable and suboptimal practice were observed in patients undergoing infusion therapy in terms of insertion and maintenance of peripheral IV catheters. Costa et al. (2022) discovered that in 470 patients who were given peripheral IV catheters, 26% developed complications that were directly caused by a lack of observance of a non-touch aseptic technique. The systematic review and meta-analysis by Marsh et al. (2024) showed that there was a correlation between high rates of preventable peripheral IV failure and infection with globally inconsistent catheter care. The inconsistent and/or non-standardized practice that the project team identified in the clinic was apparent through the previously gathered data (chart audits, electronic health records, direct observational assessments).
Flawed Processes Leading to the Practice Problem
There exists a great deal of disconnect that has been clearly documented between present infusion practice and accepted standards of practice in local, national, and global practices. The complications related to medication infusion, which are reported by 35.6 percent of the patients undergoing outpatient antimicrobial treatment via the infusion pump, suggest that the problem of infusion safety in the outpatient environment has been persistent (the work of Staples et al., 2022). Young et al. (2023) restated that with the continuously growing and evolving outpatient procedures, there is still a need to continuously work on standardizing safe practice measures to safeguard an increasingly heterogeneous group of medically vulnerable patients. As Nickel et al. (2024) showed, regularly checking the IV site with valid grading scales and applying the same aseptic technique to every catheter insertion are both obligatory components of an existing standard of safety. The 14% complication rate at the site is quite an outlier to the published rate of less than 10% in the institutes where standardization of service delivery methodology has been adopted, and hence justifies an immediate intervention.
Evidence consistently and extensively reinforces the need for the use of a structure and protocol-driven approach to administering infusions in order to reduce the risk of preventable complications when performed in outpatient settings. When Demiroğlu and Tosun (2025) added a protocolised care bundle of evidence-based practices to the use of peripheral IV catheter care, the researchers were able to show statistically significant reductions in the incidence of phlebitis when compared to those of regular care (p < 0.05). Lewis et al. (2022) state that competency-oriented training leads to greater patient safety in the clinical setting, staff members with the necessary levels of skills, and long-term sustainability of established quality improvement measures.
Jacobs (2022) found that through structured validation of competencies by standardised IV assessment regimes, the quality of IV insertions can be improved and at the same time lead to statistically significant reductions of IV-related adverse events among nursing staff. The use of standardized IV site assessment and the use of aseptic technique are identified as primary safety requirements in the outpatient infusion care (Infusion Nurses Society, 2025). The infusion therapy complications that are not addressed according to standardised protocols have a profound effect on the quality of life of patients and their further treatment of various disease processes (Van Laar et al., 2023). The evidence has all indicated the urgency of the need to implement an organized INS-aligned assessment protocol and an aseptic technique compliance bundle to seal the practice gaps identified in the project site.
Project Site
Outpatient infusion centers play a crucial role in the provision of ambulatory healthcare in a wide variety of communities. Our study set location will be a privately owned outpatient wellness and infusion center located in a suburban community in a metropolitan area. The site is targeted at adults who are medically sound and seek elective and supportive intravenous interventions at the primary ambulatory level of care (Clinical Director, personal communication, January 15, 2026). There are numerous treatment chairs in the infusion suite, which means that multiple patients can get IV treatments simultaneously (Clinical Director, personal communication, January 15, 2026). The registered nurses make up a small clinical staff at the center who are under the supervision of a qualified clinical director, who is knowledgeable in advanced infusion therapy. To develop quality improvement initiatives that are effective, understanding the structural and operational characteristics of the site where the initiative is to be implemented.
The selection of the location where you are going to carry out your doctoral quality improvement project is of crucial importance in deciding whether or not your innovation will become a success, and whether or not it can remain an effective innovation. The Center under consideration will focus on 25-35 adult patients per day. All patients will be given an infusion therapy once a week (out of 150-200 infusion sessions). Thus, the site will offer sufficient chances to make a considerable assessment of the infusion outcomes based on gathered facts (Clinical Director, personal communication, January 15, 2026).
The clinical director has also provided complete access to de-identified electronic health records of the patients under treatment in the clinic, and all the electronic templates and observational procedures required to carry out a pre-treatment assessment (Clinical Director, personal communication, January 15, 2026). The bi-weekly meetings with the stakeholders of the clinic featured registered nurses, operations coordinator, and clinic administrator, and made sure that the project was supported by all stakeholders of the organization (Clinical Director, personal communication, January 15, 2026). Moreover, the project is a first-order indication of the strategic objectives of the organization that include the enhancement of patient safety, reduction of unnecessary complications, and the quality of infusion care. Congruence between the objectives of the project and those of the center will significantly enhance the likelihood of a successful implementation and maintenance of practice change.
Current Practice Limitations and Previous Improvement Efforts
The gaps identification process of the current approach to doing things within the organization is a critical constituent in developing the evidence-based, concrete quality improvement initiatives. The current way that the facility practices is primarily reliant on the clinician’s knowledge of the practice and how the providers were orientated, and not structured through a competency validation framework (Clinical Director, personal communication, 1/15/2026). The grading of phlebitis is not done in a standardized grading scale but rather in a descriptive format, which limits the potential to be able to objectively compare and trend complication data through the use of the chart reviews (Clinical Director, personal communication, 1/15/2026). According to nursing personnel, one of the obstacles to routine recording was that reassessment prompts be added to the electronic recording template, which would help address the issue of peak volume scheduling blocks. There is no instituted quality improvement programme within the site, which deals in an orderly manner with infusion-related complications, or a standardisation of the practice of aseptic technique. The second role that the lack of a formal improvement initiative plays is to underscore the reasons as to why the evidence-based DNP project ought to be undertaken on the site.
Project Population
The first step is to define the target group to design a rigorous and meaningful quality improvement project. Registered nurses working in an outpatient infusion center that offers peripheral IV insertion and peripheral IV monitoring services will be part of the project. The same clinical role of direct patient care will apply to all nurses who will be doing IV infusion therapy at the practice site. Tegegne and colleagues (2025) found that nurses’ knowledge and clinical practices will impact the rate of peripheral IV complications in an outpatient setting. The investigators will be confident that the interventions offered will be timely and relevant by outlining the general role, duties, and clinical setting of the population.
Population Similarities and Clinical Context
Quality improvement interventions can be more internally consistent and generalizable by identifying general features of the study participants in a project. As an illustration, all nurses involved are oriented to perform the same basic clinical practices, including the insertion of peripheral IVs, observation of the IV insertion site, patient history and treatments received, and use of aseptic skills when inserting infusions. In addition, the nursing staff roles, workflows, and documentation, and interactions with patients are the same in the outpatient environment and infusion setting. Lewis et al. (2022) have shown that competency-based training programs are optimally designed in terms of how often a particular clinical population has the identified common standard skills and practice settings. The single standardised training and assessment tool can be created and applied to the whole group of subjects by recognizing common professional traits of the involved clinical population.
Inclusion and Exclusion Criteria
This will be enhanced by clear inclusion and exclusion criteria, which will give integrity to the data collected, thereby giving an overall better product and a more reliable product of the research project. The inclusion criteria used in the research project will be the following: the participant needs to currently be working as a registered nurse who is currently doing peripheral intravenous (IV) insertion and infusion monitoring in the project location. The registered nurses who have a long leave of absence, recruited after the project commencement date, and those who have no connection with peripheral intravenous (IV) care will not take part in the project. The project has 15 registered nurses working on it. The registered nurses working at the site all satisfy the inclusion criteria and thus will provide an adequate and clear pool of participants on whom to gather data. With the total number of 15 participants, an adequate number of registered nurse workforce will be represented, and the possibility of quantifying the competencies, compliance, and practice changes during the research project implementation will be strengthened.
Evidence-Based Interventions
To solve the complications that are preventable, to standardize the manner in which clinicians administer Infusions to their patients in outpatient clinics, and to have clinicians rely on the evidence as a means to inform clinical decision-making, there should be an appreciation that an evidence-based approach is a way of practicing safely. Routine and ongoing assessment of the IV site with the use of a validated grading scale along with meeting the standard for the use of Aseptic Technique is critical to promoting patient safety in all infusion settings. The application of the “Established Professional Standards” based on the results of the research is proved to be effective in terms of the impact on the safety outcomes of the patients (Nickel et al., 2024). On the other hand, Thompson et al. (2026) showed that the national PIVC Failure and Complication Rate range from 35-50%. According to Thompson, his results imply that there is still a long way to go in terms of non-adherence to the set standards of clinical competence and systematic clinical application of evidence based standards and competency. The research conducted by Thompson et al. (2026) was mainly interested in the disparity between the formulated guidelines and the standard of practice. When the professional standards are based on the selection of interventions by the clinician, what the clinician gets in his/her practice is a direct and logical correlation between the issue that he/she is applying the evidence-based practice change and outcomes that are expected of the given intervention.
Intervention One: Standardized INS-Aligned IV Site Assessment Protocol
Use of standardized methods of assessment is one of the most thoroughly proven interventions of minimizing the number of complications related to the use of peripheral IVs in a variety of clinical settings. Nickel et al. proposed that validated scales to grade phlebitis, prescribing timeframes to re-assess phlebitis and a structured electronic documentation field should be in the list of components of a safe infusion protocol (Nickel et al., 2024). Nevertheless, Paterson et al. (2022) went further by proving that not only individual assessment tools were used, but also the use of standard evidence-based guidelines and clinical practice escalation pathways greatly increased the success of first-attempt insertion and patient outcomes. Although the results obtained by Nickel et al. (2024) can be generalized to all infusion settings, they did not focus on the population that faces a challenging access to IVs; therefore, Paterson et al. (2022) decided that standard protocols are to be adopted to cater to patients with different levels of complexity linked to the IV access. Demiroglu and Tosun (2025) also substantiated the argument by showing that phlebitis was statistically significantly reduced by the implementation of a structured peripheral IV care bundle, which included standardized phlebitis assessment (p < 0.05), hence demonstrating the notion of standardization of protocols, which yield measurable and clinically significant outcomes.
Intervention Two: Aseptic Technique Compliance Bundle
Aseptic technique bundles have been a well-established, evidence-based method of preventing the occurrence of vascular access-related infections and complications associated with intravenous therapy. In their scoping review, Kent et al. (2025) concluded that the use of aseptic technique by nurses varied significantly across specific nurses and clinical environments, and standardization of this practice at the facility level was essential. But Malhi et al. (2025) did not just identify variability as authors also showed that with the application of a standardized aseptic non-touch method the training time (63%) was reduced and no catheter-related bloodstream infection was observed throughout the study period on patients who administered parenteral support at home through a standardized aseptic non-touch method. Though Maliki et al. (2025) were investigating home patients, Kent et al. (2025) was a generalised study of the different settings of clinical nursing practice, indicating that the benefits of aseptic technique standardisation are applicable to all patients, irrespective of the care setting. Nonetheless, although researches were done to determine the correlation between structured, standardized aseptic practice and decreased risk of infection, they gave good reasons why aseptic technique compliance bundle should be implemented at the project site.
Comparison and Contrast of Interventions Within Literature
The comparison of the evidence obtained in various studies justifies the logic in applying the specified interventions and assists to prove the accomplishment of the objectives described in the project. Demiroglu and Tosun (2025) preoccupied themselves with the prevention of phlebitis using bundled peripheral intravenous (IV) care and significant statistical differences were found that the number of complications linked with the insertion of an IV decreased, but Malhi et al. (2025) discovered that with the standardization of the use of the aseptic non-touch technique, there are also advantages The most comprehensive clinical model based on combining site assessment and aseptic technique as mutually supportive facets of safe infusion practice was presented by Nickel et al. (2024), whereas Paterson et al. (2022) paid more attention to building the standardization of the assessment tools and the escalation routes toward patients with challenging access. Thompson et al. (2026) summarized the views on the system level and claimed that the lack of the nationwide adoption of a standard of care on peripheral IV access (PIVC) has a significant adverse effect on a large number of human beings and further justified the need to adopt intervention strategies on a national scale rather than a national priority level. The overall effect of all the studies is to offer solid and consistent evidence on the use of a combined multicomponent intervention model as the superior one in the face of either evaluation, or aseptic practices of infusion.
Supporting Evidence for Competency-Based Training
Another strategy that is vital in ensuring and maintaining primary interventions during the implementation process is competency based training which is well structured. The findings of Ray et al. (2022) were that nurse participants had shown a significant statistical improvement in the general knowledge of the intravenous (IV) infusion therapy and the perceived self-confidence in the ability to execute IV infusion therapy following the involvement in the organized, interactive modules of education (p <0.001). On the contrary, Hawker et al. (2022) recommended that nursing training on Aseptic Technique is mostly uneven and that the scores of confidence expressed by the learners do not relate to the real level of knowledge. Nevertheless, although the report by Ray et al. (2022) proved that using interactive infusion education modules was successful in the short-term, the authors also mentioned that the methodology weaknesses of other examined studies required continuous demonstration of competency and not just one-time educational process to gain knowledge (Hawker et al., 2022). Still, Lewis et al. (2022) helped to reconcile the two sides of the paradigm as they showed that competency-based education models also necessitate the staff to exhibit the knowledge and skills that are expected to complete clinical tasks. Therefore, through skill validation checklists, visual cue cards and hands-on simulation as an element of design strategy, all 15 RN participants will attain and sustain the competency standards during each of the 4 project implementation phases.
Consistency of Practice Recommendations With Project Problem and Desired Outcomes
Quality improvement projects need to be credible by having a rational and evidence-supported connection between the literature, practice guidelines and proposed interventions. Great enhancement in patient outcomes related to early identification of complications connected to vascular access and application of clinical practice guidelines (Paterson et al., 2022). The same information offered by Yang et al., 2025 extended the analysis to the outpatient community clinics, showing that the implementation of standardized maintenance procedures on the catheters brought about quantifiable decreases in catheter-related adverse events similar to the desired results of the project. In addition, the authors cited the credibility of assessment tools and clinical escalation route as to be of utmost importance in the findings.
Instead, Yang et al. (2025) offer more overall validation that there is a need to standardize clinical practice in an attempt to optimize practice improvement but are open to all spheres of standardization to be successful. The results by Jacobs (2022) summarize the findings of Yang et al. (2025) and Paterson et al. (2022) to conclude that the implementation of competency based validation as a part of a standardized vascular access assessment program can enhance the quality of vascular access and decrease the number of adverse vascular access-related events, which is justified by the combination of competencies and standardization being viewed This unity of evidence thus confirms the plausibility that the identified interventions are logically, evidence-supported, and operationally coherent to the problem of the project, the population to be covered and the quantifiable results to be realized at the project location.
Implementation Plan for Interventions
Step-by-Step Implementation Protocol
An implementation plan has to be clear and repeatable in order to guarantee the success and fidelity of the quality improvement projects. During week one, the project Lead will finalize all of his standardized tools that will be given to the nursing staff; the INS phlebitis grading scale, iv reassessment checklist, and aseptic technique observation audit tool. In weeks two and three, competency-based training by a structured training session will be given to the 15 RNs to teach INS Standards, Phlebitis grading scale, reassessment intervals, and practice of Hands-on Aseptic Non-Touch Technique. Lewis et al. (2022) discovered that a competency-based framework can be used to ensure that staff who are shown to have competency-level skills before they can carry out independent procedures after which the practice change is deemed as long-term sustainable. The Standardized IV Site Assessment Protocol and Aseptic Technique Compliance Bundle implementation will be initiated in week four to week eight and entail application of the protocols to all the infusion encounters, weekly chart audits and regular structured observation audits will be used to gauge adherence and impediments in the workflow.
By determining the roles of each team member, a clear sense of responsibility is given to each team member; this promotes a spirit of cooperation and ensured implementation throughout the project period. The Project Lead will then be in charge of developing all standardized tools, weekly audits, training the nursing staff, outcome data collection and giving real-time feedback to nursing staff in the implementation. The Clinical Director will serve as the preceptor and site champion which will involve operational supervision and any modifications of the staff schedules in the training process and review the results of the audits in the weekly meeting with the staff. Nickel et al. (2024) observed that in case the organizations have a defined, nurse-based implementation plan where the infusion protocols are aligned to the INS, and where the organizational leadership supports the implementation of standardized care practices, the compliance rates with the standardized care practices in an outpatient environment are significantly higher. All Registered Nurses should make sure that the IV site assessment protocol as well as the bundle of aseptic technique compliance are implemented regularly by ensuring that they are applied on all encounters related to the peripheral IV infusions (within the eight-week implementation period).
Scholarly Leadership and Project Oversight
Developing a professional leadership position that demands achieving fidelity in initiatives, stakeholder interactions, and strict supervision throughout implementation. The scholar project lead would facilitate every element of implementation, such as; developing tools, staff training, arranging audits, data collection, and continuing formative data analysis of outcome measures. The preceptor will take part in a weekly meeting with the project lead to review audit findings, barriers that might come up, the workflow processes and ensure the project is timely and in line with the organizational objectives. Quality improvement programs implemented by nurses influenced the changes in adherence to the standardized IV care protocols within clinical settings in a positive way in the presence of structured leadership supervision and regular stakeholder involvement (Jacobs, 2022). Ensuring transparency by communicating with all stakeholders and team members at every stage of project implementation will guarantee the systematic flow of the project and accuracy and completeness of outcome data.
Preceptor Partnership and Collaborative Oversight
The successful partnership between the leader of the project and preceptor plays a major role in attaining the scholarly validity and operational feasibility of the quality improvement initiative. In the implementation stage, the preceptor will guide weekly on the initiative, grant the relevant permission to access audit data and electronic health record templates and facilitate communications on the activities of the project leader to nursing employees. Formative analyses of data gathered using chart audits, observation audit and competency check-offs will be conducted biweekly so that any initial patterns can be discovered and any gaps can be addressed. Through active monitoring, giving structured feedback, and assisting adherence to the protocols developed throughout quality improvement efforts demonstrated that Demiroglu and Tosun (2025) reported that significant decreases in the occurrence of infusion-related complications are still maintained in the long term. An overview of the data produced as a result of the formative analyses and the resulting outcome data will offer an idea of what went wrong with the plan that can now be corrected without violating the overall integrity of the project.
Internal and External Stakeholder Engagement
In developing a solid base and permanence of change in practice, it is highly vital to work and locate stakeholders in various levels of your organization. The clinical director, registered nurses, and operations coordinator make up internal stakeholders; and all these individuals are directly involved with the day-to-day provision of infusion care and workflow management at the project site. The internal stakeholder and project administrative champion is the clinical administrator, who offers a transitory modification in the staffing schedules during training, and also authenticates the project with the leadership of the organization. Research conducted by Jacobs (2022) shows that having visible endorsement from leadership as well as having a structured way to engage and support stakeholders will increase adherence to standardized infusion protocols and sustainability of practice change in outpatient settings. External stakeholders are the patients receiving infusion therapy. The project will eventually benefit patients undergoing infusion therapy by helping to cut down the occurrence of complications, enhancing consistency in care provision, and overall safety during the entire treatment period of the infusion treatment.
Interprofessional Team Composition and Functions
Interprofessional collaboration (Interprofessional Collaboration ICC) has been associated with quality improvement work in complex outpatient health settings, and has been shown to positively impact quality when teamwork occurs. The project ICC team members include: the Doctorate of Nursing Practice (DNP) project leader, Preceptor (Clinical Director), Registered Nurses, the Operations Coordinator, and the Clinic Administrator. Each of the members is unique and has complementary roles that are added to the project. The Operations Coordinator will play a key role in aiding the effort by offering logistical support including scheduling, staff training by ensuring that specific time is safeguarded, and to organize staff availability to conduct observation audits throughout the project. Nickel et al. (2024) report that interprofessional collaboration is essential among nursing leaders, clinical staff, and operational team members to effectively implement and follow the adherence to the standards of infusion therapy in compliance with INS standards in outpatient clinical settings. All ICC team members have distinct roles that facilitate the project at both clinical, operational and administrative tiers, thereby enabling the so-called integrated approach to implementation to take place where all the mentioned programs collaborate to reach a shared objective.
Team Member Collaboration and Communication
With the clear identification of unique roles of the individual team members in an interprofessional team, the application of systematic and continuous implementation of a project can be accomplished completely, and teams become responsible to implement outcomes during the project life cycle. The registered nurses will be the key agents in implementing the two forms of interventions as they will apply the use of the Standardized IV Site Assessment Protocol and the Aseptic Technique Compliance Bundle to each intravenous infusion they encounter. The Clinical Director will serve as the clinical expert on the project and liaison to the organization, mentor the Project Leader, review data of Formative Audit, and hold the implementation of the activities in the project accountable to patient safety priorities in the organization. Engagement of interprofessional teams that are planned and organized with clarified role expectations and leadership, as shown by Jacobs (2022) will lead to improved quality and sustainability of implementing IV standardized care improvement initiatives. The work of all interprofessional team members will make sure that the project is implemented in a clinical rigorous manner that is operationally precise and aligned with the organization in the full implementation period of eight weeks.
Data Collection, Analysis, and Desirable Outcomes
Desirable Project Outcomes
Clear targeted project outcomes are measurable indicators that define how successful quality improvement efforts are. The main aim of using standardized protocol regarding 8 weeks is to achieve at least 30 percent or more decrease in the occurrence of complications with IV infusions in non-hospital setting (i.e. it is an outpatient setting) (i.e. catheter occlusion, infiltration, phlebitis etc.). The secondary desired outcome measure is that 90 percent of the nurses will record the adherence to the IV site evaluation protocol, regularly adhere to the required adherence bundle of adherence to the aseptic technique, and provide proper and complete reporting of all infusion encounters in the Electronic Health Record. Demiroglu and Tosun (2025) demonstrated statistically significant decreases in phlebitis following adoption of structured peripheral IV care bundle within an outpatient infusion context, which supports the conclusion that multifactorial standardization process generates consistent, measurable and clinically significant improvements in the outpatient infusion context. The above-mentioned outcomes will cumulatively demonstrate that evidence-based practices systematization will enhance patient safety levels, advance the uniformity of nursing practice, and add to the long-term maintenance of quality infusion care at the location of the project.
Evaluation Criteria and Measurement Approach
There will be a need to have clear and objective assessment criteria to suggest whether the planned practice change has occurred during the implementation process. The key outcome measure that will be used to determine the infusion related complication rate will be the weekly electronic health record audit of several charts where incidences of phlebitis, infiltration and catheter occlusion will be documented in all infusion encounters. In order to determine adherence to the standardized IV site assessment protocol, a structured checklist will be applied to determine the accuracy of phlebitis grading, to determine when the physician reviewed IV sites based on standard practice and to determine whether all the needed documentation fields were filled in every IV site assessment documentation record. Nickel et al. (2024) describe the INS Phlebitis Scale as a valid, standardized instrument often applied in studies concerning infusion therapy that can be utilized to objectively rate phlebitis levels on the basis of clinical evidence like erythema, pain, edema, and palpable venous cord. By implementing equivalent and approved methods of measuring all the measurements, the outcome data obtained will be representative of the actual outcomes of the interventions, and the project results can be reputably disseminated.
Measurement Tools, Validity, and Reliability
The methods of measurement tool selection are valid, reliable and consistent in giving valid and accurate quality improvement measurement results. Therefore, the use of INS Phlebitis Scale will be used as the main measuring device to grade the presence of complications in peripheral IV site to develop an objective and standardized way of recording and comparing the intensity of complications in all infusion-related care episodes. The clinical reliability of the INS Phlebitis Scale and the content validity, has been proven by the consistent implementation of the tool in many research studies, clinical quality improvement initiatives, and clinical trials of infusion therapy on the international level (Nickel et al. 2024). The INS is publicly accessible as a professional aid and it has eliminated the necessity to seek further permission to use the corresponding tools and will enable the transparent, replicable and accessible measurement processes in the project.
Data Analysis Plan
To be able to interpret outcomes of a project and to release results on quality improvement in a meaningful way, it is necessary to have a well-defined and a suitable data analysis plan in place. Because the project sample size is 15 nurses and the data have been gathered in a weekly level of encounter in eight weeks, descriptive statistics will be the only type of analysis that will be applied to evaluate the data. The rates of complications will be calculated and displayed in percentages of the number of encounters ofweekly infusions to make baseline complication rates directly compared to the complication rate after the implementation at each measurement period. Marsh et al. (2024) revealed that descriptive measures in terms of percentages to measure the number of peripheral IV complications monitored is a simple, clinically important, and easily conveyed technique to evaluate the effectiveness of standardized infusion care interventions. By showing the outcomes data using easy means such as percentages or counts of frequency, all stakeholders, such as the nursing staff, clinical directors, and organizational leaders will easily interpret the project outcomes.
Weekly Data Tracking and Outcome Reporting
In the implementation process, data should be regularly and systematically tracked to determine the trends, track the implementation progress, and give timely feedback on making decisions that will influence the capacity to attain the desired objectives. A running data tracker will include weekly chart audits of the charts where complication rates are recorded, adherence to protocol, and documentation completeness during the eight weeks. Observational audits compliance rates will be monitored in a comparable fashion, by calculating weekly percentages of total observations done representing all bundle components, which will allow amassing trend data and providing the nursing staff with specific feedback where the need arises. Through the literature review, Jacobs (2022) demonstrated that continuous data monitoring with periodic feedback to clinical personnel will be able to increase adherence to standardized guidelines and result in long-term improvement of the IV care outcomes. The summary of all descriptive data gathered into weekly percentages of comparison and a final pre/ post implementation summary table will help in the easy organization of project outcomes; report project outcomes transparently and make it easily available to disseminate project outcomes to stakeholders and the rest of the nursing practice community.
Conceptual Model
Plan-Do-Study-Act Model Overview
One of the effective methods that systems can use to organize and implement QI (quality improvement) programs in a health care system is by using a reliable system of reference. PDSA (plan, do, study, act) is a model that is based on a series of structured phases, which is used to create test and implement quality improvements in a cyclic iterative process. Since Abuzied et al. (2023) mentioned that the PDSA is a systematic way to ameliorate a procedure by applying changes through cumulative and gradual alteration and a rapid adoption of new procedures through a clear procedure of review and reconsideration in addition to a comprehensive examination of new evidence that may influence the existing process, the methodology is quite suitable in complex health care settings. Elhihi et al. (2025) confirmed that PDSA method enhances the effectiveness, sustainability, and overall quality of QI programs in various settings by integrating PDSA methodologies and EBP (evidence-based practice) methodology to develop successful QI initiatives. The adaptable and repeatable cycle of the PDSA model, is a most appropriate method to formulate, follow up and refine the application of standardized infusion therapy protocols at the site of the clinical improvement project implementation.
Connection of PDSA to Project Goals and PICOT
Conceptual framework of the project stays in alignment with the PICOT question and thegoals; therefore, all phases of implementation will have a clear purpose, an ability to provide measurable results, and be based on evidence. The standardized INS-aligned IV site assessment protocol, the aseptic technique compliance bundle, competency training materials, and all tools used to collect data will be developed in the Plan phase of the project, and implemented before actual implementation.
During the Do phase, each of the registered nurses involved in the study (15 nurses) will receive structured competency training, and interventions will be applied uniformly to every patient who has received a peripheral IV over the project time frame (8 weeks). Pathan et al. (2024) discovered that a clinical unit efficiency increased 15 percent, 60 to 75 percent bed occupancy, after the implementation of the healthcare improvement project plans based on the PDSA phases, as well as, through process mapping, accompanied by the root cause analysis, at the conclusion of the 8-week implementation. The correlation of every stage of the PDSA cycle with the corresponding PICOT elements aids the logical development of the project towards a concrete outcome of reducing the incidence of infusion-related complications in the 8-week period of implementation.
How the PDSA Model Will Guide the Project
The PDSA Framework also offers an operational and systematic roadmap to quality improvement implementation, monitoring, and refinement during the duration of the project. Data collection will be addressed during the Study phase through conducting weekly chart audit, observation audit and check-off competency completion rate to identify the outcomes of the interventions expected and to identify the barriers created.
Abuzied et al. (2023) acknowledge that the Study phase of the PDSA Cycle is the most important phase in the analysis of process and outcome data to identify potential process improvements by contrasting them with pre-defined benchmarks at each interval. Information about the formative analyses will also guide the re-design of workflow challenges, documentation disparity, the improvement of aseptic technique compliance, and the maintenance of all nursing staff Protocol conformance by the rest of the implementation phase in the Act phase. Due to the cyclical nature of the PDSA model, real-time data will continually change the project response ensuring continued refining of the interventions to promote patient safety and sustainable practices.
PDSA Model in Similar Healthcare Improvement Circumstances
The PDSA model has been widely used and efficient in successfully delivering healthcare quality improvement initiatives. An example by Elhihi et al. (2025) could actually prove that PDSA methodology as a part of the use of evidence-based practice could reduce central line infection rates of 1.37 infections to 0.62 infections per 1000 patient days in an ICU. Multimodal interventions that are directed by PSDA have the potential to yield tangible and quantifiable results concerning infection prevention.
Likewise, Pathan et al. (2024) applied the PDSA cycle to a chemotherapy daycare unit to enhance bed utilization efficiency by improving processes using process improvement tools such as structured process mapping, root cause analysis and subsequent improvement of interventions across multiple PDSA cycles. Moreover, Abuzied et al. (2023) advocate PDSA methodology as a means to produce guidelines and protocols, interact with interdisciplinary stakeholders and help maintain continuous quality improvement of multifaceted and intricate healthcare processes. The successful outcomes of the PDSA in the number of infection-related complications reduction and the standardization of care in similar clinical situations are the evidence of the appropriateness of PDSA to be used as the framework of the quality improvement project in outpatient infusion.
Methodology, Budget, and Ethical Considerations
Project Methodology and Design
The project methodology has been established to offer a clear outline of how the quality improvement project will be implemented with integrity, transparency and rigor across the project timeline. This project is planned as a quality improvement project which will make use of a pre-post implementation framework, to monitor the shortcomings in relation to infusion-related complications which had been experienced during the eight weeks of implementation as opposed to the pre-implementation deficiency rate of each of the infusion related complications. The project presupposes the entire involvement of 15 registered nurses (RNs), the stable organisational support of the Clinical Director and the fact that the diagnostic indicators of infusion encounters will not change during the project implementation phase.
Marsh et al. (2024) hypothesise that with the use of the pre-post concept and regular data collection procedures, quality improvement projects generate meaningful and reliable data on clinical outcomes when comparing pre-implementation and post-implementation using data collected as per peripheral intravenous line care. Since the aggregate and de-identified project data is used to infuse the encounters of the project with the development of professional competencies and the project does not involve actual patients, the project will not require formal institutional review board (IRB) approval, although the principles of the human subject’s protection will be observed in all project cases.
Project Limitations and Mitigation Strategies
Credibility and integrity of the quality improvement findings and the broader implications demand that project limitations are brought to the fore in an open way. The restriction of findings to other infusion care locations, as well as to much larger nurse populations, is the project’s principal restriction: the size of the sample of nurses at one outpatient location is limited to fifteen. Auditing bias associated with an aseptic method, irregularities in the electronic health record documentation and the possibility of disturbances to employee schedules during the eight-week implementation period are other limiting factors.
Demiroglu and Tosun (2025) admitted the limitations of contextual limitations of quasi-experimental quality improvement study based on one site, and affirmed the application of homogeneous criteria in audits and formal monitoring procedures to reduce the level of bias and increase the reliability of data. Strategies that will help alleviate the constraints will be the use of a consistent audit tool on all audits, observation by all scheduling blocks, continuous feedback to staff and open communication between the preceptor and the staff to enable prompt response to hurdles that occur during the implementation period.
Project Budget
In order to develop a successful and all-inclusive project in budget development, to identify, allocate the necessary resources before, during and after implementation. Staff costs are the largest part of the project budget because it will cover how much time will be used by the nursing staff in the competency training sessions that will last 2 weeks; attend weekly audits; and occupy in biweekly stakeholder meetings all of which will occur within a 8 weeks period. Other budget items will be the price of supplies to be used as printed IV site assessment checklists; phlebitis grading reference cards; visual cues of aseptic technique to be used at infusion stations; and competency check-off forms to each of the nurses who park.
Jacobs (2022) has clarified that the presence of the staff time as a budgeted project element, aids in determining how much of the actual costs of operations goes into enabling competency-based quality improvement programs to be applied in clinical practice environments. The clinical director and operations coordinator will organize the modification of the electronic health records (EHR) system, including the addition of new fields to the system with standardised reassessment prompts and structured documentation templates, to implement in an efficient and effective manner to support the implementation process accordingly within the constraints of the budget.
Health Insurance Portability and Accountability Act (HIPAA) Compliance and Data Security
Whenever a quality improvement project is planned that includes clinical data, full compliant to HIPAA regulations and proper secure data protocols should always be followed. During the process of enhancing your quality improvement project, audit information, gathered through chart audits/clinical records will not contain any access, store, or report individually identifiable information (patient data) pertaining to any patient in the entire duration of the project, only de-identified, and aggregate encounter data.
Besides this, any project document, such as the weekly audit records, competency check-off sheets, and observation audit will be stored on an encrypted (protected by a password), project leader only laptop at all project stages, both at the beginning and end of the project. Elhihi et al. (2025) recommend that should all data be stored with complete anonymity and security during quality improvement initiatives to protect the privacy of patients and ensure that the data stays within the limits of institutional and federal data security regulations. All hard copy data documents (such as printed audit document, competency checklists) shall be kept locked away in cabinets at the project site which can be accessed only by the project lead and preceptor with further precautions taken to maintain data confidentiality and security at all times during the project.
Project Timeline
Implementation Timeline and Work Plan
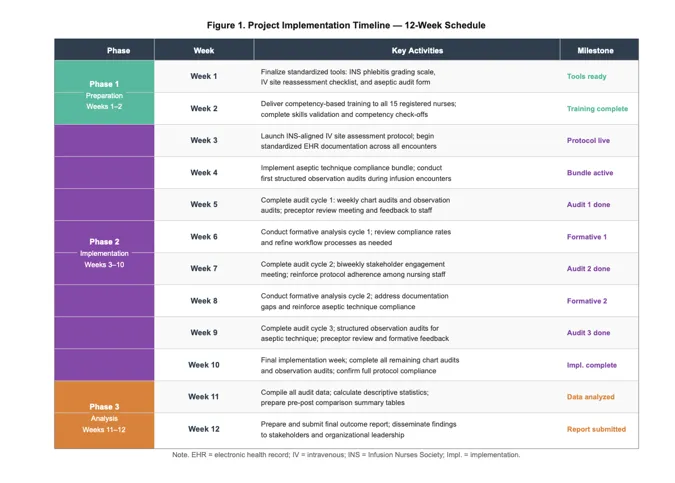
A project timeline offers a framework and forecasts on how productive implementation should be to ensure everything in a project is accomplished within a given time frame. The project schedule of the project is twelve (12) weeks, which will be divided into three (3) phases: preparation phase, which will last two (2) weeks, implementation phase, which will last eight (8) weeks and data analysis and dissemination phase, which will last two (2) weeks.
Pathan et al. (2024) state that a PDSA framework that helps to organize quality improvement projects into clear and sequential stages (as seen in) aids in improving productivity, stakeholder participation, and enables more measurable results to be achieved in specific timeframes. The weekly milestones set in advance of each of the subsequent project steps: Tool finalization, training of staff, protocol implementation, chart audit, observation Audit, Formative Analysis and Final Outcome Reporting (each of which will take place once/week over a total 12 weeks) give a clear and concise week-by-week schedule. Timelines shall be employed to make sure that the parts of the project occur in an organized fashion and establish any potential impediments to implementation wholeness ahead of time.
Figure 1
Project Implementation Timeline
Practicum Hours Plan of Action
To fulfill the requirements of advanced clinical scholarship and professional competence during the DNP program, students have to complete 1,000 hours of practicum hours working on the course assignments in 4 courses (NURS-FPX9000, NURS-FPX9020, NURS-FPX9030, and NURS-FPX9040). The 1,000 hours will be covered in the core courses, and will be connected together by individual course-specific projects concerning the Infusion Safety Quality Improvement Initiative.
Lewis et al. (2022) substantiated the existence of competency-based structure in practicum experience to improve your clinical leadership capacity and offers an evidence-based practice and quality improvement project management methodology to advanced nursing practice. Part of the activities that will occur during the DNP program include: literature review, site evaluation, stakeholders engagement, protocol elaboration, staff education/training, data gathering, audit monitoring, formative assessment and the ultimate outcome dissemination. The practicum hour plan will cover how all the projects will be recorded during the DNP program and also tabulates the different contributions of each individual class work (project) to the total 1,000 hours.
Table 1
DNP 1,000 Hour Practicum Plan of Action
DNP 1,000 Practicum Hour Plan Of Action | |||
Transfer Hours – Please indicate if they have been approved or submitted. | |||
DNP Project Hours | Total from core courses. | 1000 | |
Hours from NURS 9000. | 100 | ||
Projected hours from NURS9010. | 100 | ||
Practicum Hours Include a description of activity and estimated hours. Add additional rows as needed. | Course | Activity | Planned hours |
NURS9000 | Literature review and topic identification for infusion safety project | 30 | |
Practice site identification, preceptor meetings, baseline data review | 30 | ||
CITI training completion and topic report writing | 40 | ||
NURS9020 | Project proposal development and submission for mentor review | 50 | |
Stakeholder engagement meetings and needs assessment at project site | 50 | ||
Development of INS-aligned IV site assessment protocol and tools | 50 | ||
Development of aseptic technique compliance bundle and audit checklist | 50 | ||
Preceptor collaboration meetings and project planning documentation | 50 | ||
IRB/ethics review preparation and HIPAA compliance planning | 50 | ||
NURS9030 | Delivery of competency-based training to all 15 registered nurses | 60 | |
Implementation of INS-aligned IV site assessment protocol at practice site | 80 | ||
Implementation of aseptic technique compliance bundle across all encounters | 80 | ||
Weekly EHR chart audits and phlebitis grading compliance monitoring | 60 | ||
Structured observation audits for aseptic technique during infusion encounters | 60 | ||
Formative analyses and biweekly preceptor review meetings | 30 | ||
Total Practicum Hours | 1000 | ||
Conclusion
This quality improvement project aims to decrease adult patients receiving outpatient infusion therapy complications due to infusion therapy by instituting two major interventions within the project; a standardized INS-aligned IV site assessment and documentation protocol and an aseptic competence compliance bundle with competency-based training. The interventions will be carried out in a 12-week period at a privately owned outpatient infusion center. During the implementation, the data will be collected by means of audit of the charts weekly and planned observation audit, processed and reported to the stakeholders with the help of descriptive statistics. In general, the introduction of the proposal would enhance patient safety, competency of the nursing staff, documentation accuracy, and replicate an evidence-based model that would standardize the care of infusion in the outpatient care unit using a PDSA conceptual framework and empirical literature to justify clinical significance and quantifiable practice deficiencies based on a baseline chart audit with a complication rate of fourteen percent among 15 registered nurses.
Step By Step Instructions To Write
NURS FPX 9010 Assessment 2
Contact us to receive step-by-step instructions.
Instructions File For
NURS FPX 9010 Assessment 2
Contact us to get the instruction file.
Scoring Guide for
NURS FPX 9010 Assessment 2
Contact us to get the scoring guide.
References For
NURS FPX 9010 Assessment 2
Abuzied, Y., Alshammary, S. A., Alhalahlah, T., & Somduth, S. (2023). Using FOCUS-PDSA quality improvement methodology model in healthcare: Process and outcomes. Global Journal on Quality and Safety in Healthcare, 6, 70–72. https://doi.org/10.36401/JQSH-22-19
Beaudart, C., Witjes, M., Rood, P., & Hiligsmann, M. (2023). Medication administration errors in the domain of infusion therapy in intensive care units: A survey study among nurses. Archives of Public Health, 81, e23. https://doi.org/10.1186/s13690-023-01041-2
Calderwood, M. S., Anderson, D. J., Bratzler, D. W., Dellinger, E. P., Garcia, H. S., Maragakis, L. L., Nyquist, A. C., Perkins, K. M., Preas, M. A., Saiman, L., Schaffzin, J. K., Schweizer, M., Yokoe, D. S., & Kaye, K. S. (2023). Strategies to prevent surgical site infections in acute-care hospitals: 2022 update. Infection Control & Hospital Epidemiology, 44(5), 695–720. https://doi.org/10.1017/ice.2023.67
Costa, P. S., Paiva-Santos, F., Sousa, L. B., Bernardes, R. A., Ventura, F., Fearnley, W. D., Oliveira, A., Parreira, P., Vieira, M., & Graveto, J. (2022). Nurses’ practices in the peripheral intravenous catheterization of adult oncology patients: A mix-method study. Journal of Personalized Medicine, 12(2), e151. https://doi.org/10.3390/jpm12020151
Demiroğlu, T., & Tosun, N. (2025). The effect of evidence-based care bundle application in the prevention of peripheral venous catheter-related phlebitis development (quasi-experimental study). Global Nursing Insights, 12(3), 245–256. https://doi.org/10.31125/globnursinsights.1721672
Elhihi, E., Lafi, K., Alahmadi, M., Al-theiba, M., Abdul Rahman, A., Maghrabi, N., Mizi, S., Alsulami, H., Altambkti, M., & Rumbo, T. (2025). Integrating evidence-based practice with PDSA methodology for the reduction of central line associated blood stream infection in intensive care unit. Worldviews on Evidence-Based Nursing. https://doi.org/10.1111/wvn.70096
Feng, T., Hu, L., Yang, Y., Du, C., & Li, J. (2025). Effective strategies for cultivating rapid response, team collaboration, and stress resistance in emergency standardized training nurses during real rescue. Frontiers in Medicine, 12, 1–7. https://doi.org/10.3389/fmed.2025.1683359
Hawker, C., Gould, D., Courtenay, M., & Edwards, D. (2022). Undergraduate nursing students’ education and training in aseptic technique: A mixed methods systematic review. Journal of Advanced Nursing, 78(1), 63–77. https://doi.org/10.1111/jan.14974
Infusion Nurses Society. (2025). Infusion therapy standards of practice. https://www.ins1.org/publications/infusion-therapy-standards-of-practice/
Jacobs, L. (2022). Peripheral intravenous catheter insertion competence and confidence in medical/surgical nurses. Journal of Infusion Nursing, 45(6), 306–319. https://doi.org/10.1097/nan.0000000000000487
Kent, H. M., Dawson, S. A., Lewis, J. M., & Mitchell, B. G. (2025). Aseptic technique in clinical nursing settings: A scoping review. Journal of Hospital Infection, 165, 171–180. https://doi.org/10.1016/j.jhin.2025.08.007
Lewis, L. S., Rebeschi, L. M., & Hunt, E. (2022). Nursing education practice update 2022: Competency-based education in nursing. SAGE Open Nursing, 8(1). https://doi.org/10.1177/23779608221140774
Malhi, H., Fitzpatrick, N., Lewis, D., Williams, V., Woodham, D., & Fletcher, J. (2025). Comparison of traditional aseptic technique versus standard aseptic non-touch technique (ANTT) in training patients to manage home parenteral support: A single centre cohort study. Clinical Nutrition ESPEN, 68, 134–139. https://doi.org/10.1016/j.clnesp.2025.05.008
Marsh, N., Larsen, E., Ullman, A., Cooke, M., Chopra, V., Ray-Barruel, G., & Rickard, C. M. (2024). Peripheral intravenous catheter infection and failure: A systematic review and meta-analysis. International Journal of Nursing Studies, 151(1), e104673. https://doi.org/10.1016/j.ijnurstu.2023.104673
Nickel, B., Gorski, L., Kleidon, T., Kyes, A., DeVries, M., Keogh, S., Meyer, B., Sarver, M. J., Crickman, R., Ong, J., Clare, S., & Hagle, M. E. (2024). Infusion therapy standards of practice, 9th edition. Journal of Infusion Nursing, 47(1), 1–285. https://doi.org/10.1097/nan.0000000000000532
Paterson, R. S., Schults, J. A., Slaughter, E., Cooke, M., Ullman, A., Kleidon, T. M., & Keijzers, G. (2022). Peripheral intravenous catheter insertion in adult patients with difficult intravenous access: A systematic review of assessment instruments, clinical practice guidelines and escalation pathways. Emergency Medicine Australasia, 34(6), 862–870. https://doi.org/10.1111/1742-6723.14069
Pathan, A., Joshi, M., & Lewis, S. (2024). Utilizing the PDSA cycle to achieve optimal bed utilization and improve the efficiency of a chemotherapy day care unit. Health Services Research and Managerial Epidemiology. https://doi.org/10.1177/23333928241253783
Ray, S. R., Taylor, E., Sherrill, K. J., Steinheiser, M. M., & Berndt, D. L. (2022). Effect of infusion therapy interactive modules on nursing student’s knowledge and self-confidence. Teaching and Learning in Nursing, 17(1), 109–112. https://doi.org/10.1016/j.teln.2021.10.006
Staples, J. A., Ho, M., Ferris, D., Hayek, J., Liu, G., Tran, K. C., & Sutherland, J. M. (2022). Outpatient versus inpatient intravenous antimicrobial therapy: A population-based observational cohort study of adverse events and costs. Clinical Infectious Diseases, 75(11), 1921–1929. https://doi.org/10.1093/cid/ciac298
Tegegne, B., Checkole, D., Shumye, M., Zeru, M., Yalew, Z., Ademe, S., Shiferaw, M., & Edmealem, A. (2025). Knowledge, practice, and factors affecting peripheral intravenous catheters among nurses working in Dessie City public hospitals. BMC Nursing, 24(1). https://doi.org/10.1186/s12912-025-03484-0
Thompson, J., Steinheiser, M. M., Hotchkiss, J. B., Davis, J., DeVries, M., Frate, K., Helm, R., Jungkans, C. W., Kakani, S., Lau, S., Lindell, K., Landrum, K. M., McQuillan, K. A., Shannon, D. J., Wuerz, L., & Pitts, S. (2026). Standards of care for peripheral intravenous catheters: Evidence-based expert consensus. Journal of the Association for Vascular Access, 8–19. https://doi.org/10.2309/JAVA-D-24-00011
Van Laar, T., Chaudhuri, K. R., Fujioka, S., Kassubek, J., Muñoz, E., Odin, P., Poewe, W., Sensi, M., Storch, A., Trošt, M., & Antonini, A. (2023). Infusion therapies in the treatment of Parkinson’s disease. Journal of Parkinson’s Disease, 13(5). https://doi.org/10.3233/JPD-225112
Wolie, Z. T., Roberts, J. A., Gilchrist, M., McCarthy, K., & Sime, F. B. (2024). Current practices and challenges of outpatient parenteral antimicrobial therapy: A narrative review. Journal of Antimicrobial Chemotherapy, 79(9), 2083–2102. https://doi.org/10.1093/jac/dkae177
Yang, Z., Fang, F., Wan, S., Gu, Y., Xu, D., Sheng, Y., & Xing, H. (2025). The practical effect of “standardized mode” in the construction of community venous catheter maintenance specialty nursing clinics. Frontiers in Health Services, 5, 1–6. https://doi.org/10.3389/frhs.2025.1680673
Young, S., Osman, B., & Shapiro, F. E. (2023). Safety considerations with the current ambulatory trends: More complicated procedures and more complicated patients. Korean Journal of Anesthesiology, 76(5), 400–412. https://doi.org/10.4097/kja.23078
Appendix For
NURS FPX 9010 Assessment 2
Appendix A
Nomenclature
Term / Abbreviation | Definition |
IV (Intravenous) Therapy | Administration of fluids, medications, or nutrients directly into a patient’s vein using a catheter |
Peripheral IV (PIV) Catheter | A small, short-term catheter inserted into a peripheral vein, typically in the arm or hand, for infusion therapy |
Infusion-Related Complications | Adverse events associated with IV therapy including phlebitis, infiltration, infection, occlusion, or extravasation |
Phlebitis | Inflammation of a vein caused by mechanical, chemical, or infectious irritation, often associated with IV catheter use |
INS Phlebitis Scale | A validated standardized tool used to grade phlebitis severity based on clinical signs including erythema, pain, edema, and palpable venous cord |
Infiltration | Accidental leakage of IV fluid or medication into surrounding tissue due to catheter displacement or vein rupture |
Extravasation | Leakage of a vesicant or irritant medication into surrounding tissue, capable of causing tissue damage or necrosis |
Occlusion | Partial or complete blockage of an IV catheter that interrupts infusion flow and may require catheter reinsertion |
Aseptic Technique | A set of specific practices and procedures performed to prevent contamination and infection during clinical procedures |
ANTT (Aseptic Non-Touch Technique) | A standardized aseptic practice framework that prevents contamination of key parts and key sites during clinical procedures |
Hub Disinfection | The process of cleaning the IV catheter hub or needleless connector using an antiseptic agent for a defined scrub duration prior to access |
INS (Infusion Nurses Society) | A professional nursing organization that establishes evidence-based standards of practice for infusion therapy globally |
INS Standards of Practice | Evidence-based guidelines established by INS to promote safe, effective, and consistent infusion therapy practices (9th ed., 2024) |
Competency-Based Training | A structured training approach that ensures staff demonstrate required skills and knowledge before performing clinical procedures independently |
IV Site Assessment Protocol | A standardized set of procedures for evaluating IV insertion sites for complications including regular inspection, documentation, and phlebitis grading |
QI (Quality Improvement) | A systematic, data-driven initiative aimed at improving patient care processes, outcomes, and safety within a healthcare setting |
PDSA (Plan-Do-Study-Act) | A cyclical quality improvement framework used to test, evaluate, and refine practice changes through structured sequential phases |
PICOT | A clinical question framework representing Population, Intervention, Comparison, Outcome, and Timeframe used to guide evidence-based projects |
EHR (Electronic Health Record) | A digital version of a patient’s medical record used to document clinical assessments, interventions, and outcomes |
DNP (Doctor of Nursing Practice) | A terminal practice-focused doctoral degree in nursing that prepares advanced practice nurses for leadership in clinical practice and quality improvement |
HIPAA | Health Insurance Portability and Accountability Act; federal legislation protecting the privacy and security of patient health information |
PIV (Peripheral Intravenous) | Refers to intravenous access established in a peripheral vein, as opposed to central venous access |
Baseline Data | Pre-intervention data collected to establish the current state of practice against which post-intervention outcomes are compared |
Descriptive Statistics | Basic statistical measures including frequencies, percentages, and means used to summarize and describe data in quality improvement projects |
Formative Analysis | Ongoing analysis conducted during project implementation to monitor progress, identify barriers, and refine interventions in real time |
Appendix B
Evidence Matrix Table
Reference | Tag | Notes |
Nickel, B., Gorski, L., Kleidon, T., Kyes, A., DeVries, M., Keogh, S., Meyer, B., Sarver, M. J., Crickman, R., Ong, J., Clare, S., & Hagle, M. E. (2024). Infusion therapy standards of practice, 9th edition. Journal of Infusion Nursing, 47(1), 1–285. https://doi.org/10.1097/nan.0000000000000532 | Practice Problem; Intervention; Guidelines | Research Question: What are the evidence-based clinical standards for infusion therapy? Methodology:Expert consensus and systematic review. Analysis:Synthesis of best practices for aseptic technique and IV site assessment. Results: Provides gold standard protocols for PIVC care. Conclusions: Adherence to INS standards is fundamental to patient safety. Implications for Future Research: Evaluate real-world adherence rates to INS standards. Implications for Future Practice: All infusion nurses should use INS-aligned protocols. |
Demiroğlu, T., & Tosun, N. (2025). The effect of evidence-based care bundle application in the prevention of peripheral venous catheter-related phlebitis development. Global Nursing Insights, 12(3), 245–256. https://doi.org/10.31125/globnursinsights.1721672 | Practice Problem; Intervention; Outcomes | Research Question: Does an evidence-based care bundle reduce phlebitis rates in peripheral venous catheters? Methodology: Quasi-experimental study comparing care bundle vs. routine care. Analysis:Comparison of phlebitis incidence and catheter dwell time. Results: Significant reduction in phlebitis rates in the intervention group (p < 0.05). Conclusions:Standardized bundles significantly improve vascular outcomes. Implications for Future Research: Larger multicenter trials recommended. Implications for Future Practice: Bundle interventions should be standard in all infusion settings. |
Marsh, N., Larsen, E., Ullman, A., Cooke, M., Chopra, V., Ray-Barruel, G., & Rickard, C. M. (2024). Peripheral intravenous catheter infection and failure: A systematic review and meta-analysis. International Journal of Nursing Studies, 151(1), e104673. https://doi.org/10.1016/j.ijnurstu.2023.104673 | Practice Problem; Baseline; Outcomes | Research Question: What are the global rates of PIVC failure and infection? Methodology: Systematic review and meta-analysis. Analysis: Aggregated data on catheter failure, phlebitis, and infiltration rates. Results:High rates of avoidable catheter failure due to inconsistent care practices. Conclusions: Inconsistent care practices drive preventable complications globally. Implications for Future Research: More prospective studies on standardized PIVC protocols needed. Implications for Future Practice: Reinforces need for standardized IV site assessment and aseptic technique. |
Jacobs, L. (2022). Peripheral intravenous catheter insertion competence and confidence in medical/surgical nurses. Journal of Infusion Nursing, 45(6), 306–319. https://doi.org/10.1097/nan.0000000000000487 | Practice Problem; Intervention; Training | Research Question: How do competence and confidence levels affect PIVC safety among nurses? Methodology: Quantitative descriptive study of medical/surgical nurses. Analysis: Assessment of self-reported confidence vs. objective competency scores. Results: Gap identified between general practice and technical competence. Conclusions: Structured training is required to bridge the competence gap. Implications for Future Research: Longitudinal studies on competency retention recommended. Implications for Future Practice: Validates need for structured competency training in the PICOT intervention. |
Beaudart, C., Witjes, M., Rood, P., & Hiligsmann, M. (2023). Medication administration errors in the domain of infusion therapy in intensive care units. Archives of Public Health, 81, 23. https://doi.org/10.1186/s13690-023-01033-y | Practice Problem; Gap | Research Question: What are nurses’ perceptions of medication administration errors during infusion therapy? Methodology: Cross-sectional digital survey among 373 ICU nurses. Analysis: Frequency and severity of perceived medication errors analyzed. Results: High patient-nurse ratios and communication gaps significantly increase MAE risk. Conclusions:Nurses perceive most medication administration errors as preventable. Implications for Future Research:Future research should examine systemic interventions to reduce MAEs. Implications for Future Practice:Staffing ratios and communication protocols must be addressed to reduce errors. |
Wolie, Z. T., Roberts, J. A., Gilchrist, M., McCarthy, K., & Sime, F. B. (2024). Current practices and challenges of outpatient parenteral antimicrobial therapy: A narrative review. Journal of Antimicrobial Chemotherapy, 79(9), 2083–2102. https://doi.org/10.1093/jac/dkae177 | Practice Problem; Gap | Research Question: What are current global OPAT practices and challenges? Methodology: Narrative review of global OPAT literature. Analysis: Synthesis of OPAT models, complications, and monitoring requirements. Results: Device complications and inconsistent monitoring are persistent global challenges. Conclusions: Standardization is essential to optimize outpatient infusion services. Implications for Future Research: Future research should focus on mitigating device-related complications. Implications for Future Practice: OPAT programs require structured monitoring and standardized protocols. |
Staples, J. A., Ho, M., Ferris, D., Hayek, J., Liu, G., Tran, K. C., & Sutherland, J. M. (2022). Outpatient versus inpatient intravenous antimicrobial therapy. Clinical Infectious Diseases, 75(11), 1921–1929. https://doi.org/10.1093/cid/ciac298 | Practice Problem; Gap | Research Question: What are adverse event rates and costs in outpatient IV antimicrobial therapy? Methodology: Retrospective observational cohort study over five years. Analysis: Cumulative adverse events and healthcare costs compared over 90 days. Results:Adverse events occurred in 35.6% of OPAT patients with significant cost savings. Conclusions: OPAT is associated with similar adverse events but substantially lower costs than inpatient care. Implications for Future Research: More research on safety protocols for outpatient IV programs is needed. Implications for Future Practice: Supports expansion of OPAT with structured safety frameworks. |
Costa, P. S., Paiva-Santos, F., Sousa, L. B., Bernardes, R. A., Ventura, F., Fearnley, W. D., Oliveira, A., Parreira, P., Vieira, M., & Graveto, J. (2022). Nurses’ Practices in the Peripheral Intravenous Catheterization of Adult Oncology Patients: A Mix-Method Study. Journal of Personalized Medicine, 12(2), e151. https://doi.org/10.3390/jpm12020151 | Practice Problem; Gap | Research Question: What are current nursing practices in PIVC insertion and maintenance in oncology settings? Methodology: Two-phase mixed-methods observational and focus group study. Analysis:Observation of practices and nurse perceptions across clinical encounters. Results: 26% complication rate directly linked to poor aseptic non-touch technique adherence. Conclusions: Significant practice variability requires targeted clinical intervention. Implications for Future Research: Future studies should test specific aseptic interventions in oncology settings. Implications for Future Practice: ANTT standardization should be implemented across all IV catheter settings. |
Young, S., Osman, B., & Shapiro, F. E. (2023). Safety considerations with the current ambulatory trends. Korean Journal of Anesthesiology, 76(5), 400–412. https://doi.org/10.4097/kja.23078 | Practice Problem; Gap | Research Question: What safety concerns arise with increasingly complex outpatient procedures? Methodology: Narrative review of ambulatory safety literature. Analysis: Review of patient selection criteria, safety standards, and ambulatory outcomes. Results:Complex outpatient patients require ongoing standardization of safety practices. Conclusions:Continuing procedural shifts require prospective outcomes research to ensure patient safety. Implications for Future Research: Prospective studies on outpatient safety standardization are urgently needed. Implications for Future Practice: Supports need for standardized infusion safety protocols in outpatient ambulatory settings. |
Kent, H. M., Dawson, S. A., Lewis, J. M., & Mitchell, B. G. (2025). Aseptic technique in clinical nursing settings: A scoping review. Journal of Hospital Infection, 165, 171–180. https://doi.org/10.1016/j.jhin.2025.08.007 | Practice Problem; Gap; Intervention | Research Question: What is the current evidence on aseptic technique definitions and application in clinical nursing? Methodology: Scoping review aligned with Joanna Briggs Institute guidelines. Analysis: Mapping of literature on asepsis terminology and application across 31 studies. Results: Significant variation in aseptic technique definitions and practice across nurses and settings. Conclusions: Standardization of aseptic terminology and practice is urgently needed globally. Implications for Future Research: Larger programs of research on aseptic technique implementation are required. Implications for Future Practice: Facility-level standardization of aseptic practice is essential for infection prevention. |
Literature Review References
Reference | Tag | Notes |
Lewis, L. S., Rebeschi, L. M., & Hunt, E. (2022). Nursing education practice update 2022: Competency-based education in nursing. SAGE Open Nursing, 8(1). https://doi.org/10.1177/23779608221140774 | Intervention; Training | Research Question: What is the current status of competency-based training in nursing practice? Methodology: Practice update and literature review of training frameworks. Analysis: Review of competency-based models across clinical nursing settings. Results: Competency-based training ensures clinical safety and improves patient outcomes. Conclusions: Moving toward structured competency models is essential for modern nursing. Implications for Future Research: More research on long-term competency retention outcomes is needed. Implications for Future Practice: Supports the pedagogical framework of the competency training intervention. |
Yang, Z., Fang, F., Wan, S., Gu, Y., Xu, D., Sheng, Y., & Xing, H. (2025). The practical effect of “standardized mode” in the construction of community venous catheter maintenance specialty nursing clinics. Frontiers in Health Services, 5, 1–6. https://doi.org/10.3389/frhs.2025.1680673 | Intervention; Outcomes | Research Question: How does a standardized mode of care affect catheter maintenance in outpatient community clinics? Methodology: Comparative study tracking complication rates and maintenance quality. Analysis: Pre and post comparison of catheter-related complications. Results: Standardized protocols led to fewer catheter-related complications in outpatient settings. Conclusions: Standardization in outpatient settings is feasible and clinically effective. Implications for Future Research: Multicenter studies recommended to confirm generalizability of findings. Implications for Future Practice: Supports outpatient infusion aspect of the PICOT intervention. |
Paterson, R. S., Schults, J. A., Slaughter, E., Cooke, M., Ullman, A., Kleidon, T. M., & Keijzers, G. (2022). Peripheral intravenous catheter insertion in adult patients with difficult intravenous access. Emergency Medicine Australasia, 34(6), 862–870. https://doi.org/10.1111/1742-6723.14069 | Intervention; Assessment | Research Question: What assessment instruments exist for identifying and managing patients with difficult IV access? Methodology: Systematic review using multiple databases with quality appraisal tools. Analysis: Quality appraisal of 24 DIVA assessment instruments and clinical practice guidelines. Results: Adopting consistent evidence-based CPGs significantly improves clinical outcomes. Conclusions:Consensus and standardization of DIVA resources is urgently limited and needed. Implications for Future Research:Consensus studies on standardized DIVA tools are needed. Implications for Future Practice: Assessment tool standardization should be adopted in all peripheral IV settings. |
Thompson, J., Steinheiser, M. M., Hotchkiss, J. B., Davis, J., DeVries, M., Frate, K., Helm, R., Jungkans, C. W., Kakani, S., Lau, S., Lindell, K., Landrum, K. M., McQuillan, K. A., Shannon, D. J., Wuerz, L., & Pitts, S. (2026). Standards of care for peripheral intravenous catheters: Evidence-based expert consensus. Journal of the Association for Vascular Access.https://doi.org/10.2309/JAVA-D-24-00011 | Intervention; Guidelines | Research Question: What are the current consensus standards for peripheral intravenous catheter care? Methodology: Multidisciplinary expert consensus with multidisciplinary and multi-organizational collaboration. Analysis: Synthesis of current PIVC standards from multiple professional nursing organizations. Results: PIVC failure rates of 35–50% reflect a fundamental lack of clinician foundational knowledge. Conclusions: Consistent high-quality PIVC care is achievable through standardization of practice. Implications for Future Research: Future research should assess impact of standardized PIVC education programs on outcomes. Implications for Future Practice:All clinical settings should adopt consistent evidence-based PIVC care standards. |
Malhi, H., Fitzpatrick, N., Lewis, D., Williams, V., Woodham, D., & Fletcher, J. (2025). Comparison of traditional aseptic technique versus standard aseptic non-touch technique in training patients. Clinical Nutrition ESPEN, 68, 134–139. https://doi.org/10.1016/j.clnesp.2025.05.008 | Intervention; Aseptic Technique | Research Question: Does ANTT reduce CRBSI and training time compared to traditional aseptic technique? Methodology: Single-centre cohort study comparing two groups from January to December 2024. Analysis:Comparison of training hours and CRBSI episodes between technique groups. Results: ANTT reduced training time by 66% and resulted in zero CRBSI episodes. Conclusions:ANTT is safe, effective, and significantly more efficient than traditional aseptic technique. Implications for Future Research: Larger randomized studies on ANTT in various clinical settings are recommended. Implications for Future Practice: ANTT should replace traditional aseptic technique in infusion therapy training programs. |
Hawker, C., Gould, D., Courtenay, M., & Edwards, D. (2022). Undergraduate nursing students’ education and training in aseptic technique: A mixed methods systematic review. Journal of Advanced Nursing, 78(1), 63–77. https://doi.org/10.1111/jan.14974 | Intervention; Training | Research Question: What is the effectiveness of aseptic technique education in undergraduate nursing programs? Methodology: Mixed-methods systematic review using Joanna Briggs Institute methodology. Analysis: Critical appraisal of 27 studies on aseptic technique education from 1996 to 2020. Results: Students’ knowledge and competency in aseptic technique were often poor despite reported confidence. Conclusions: Education and training in aseptic technique must be improved significantly. Implications for Future Research: More methodologically rigorous studies on teaching methods are urgently needed. Implications for Future Practice: Ongoing structured training should be mandatory for maintaining aseptic competency. |
Ray, S. R., Taylor, E., Sherrill, K. J., Steinheiser, M. M., & Berndt, D. L. (2022). Effect of infusion therapy interactive modules on nursing student’s knowledge and self-confidence. Teaching and Learning in Nursing, 17(1), 109–112. https://doi.org/10.1016/j.teln.2021.10.006 | Intervention; Training | Research Question: Do interactive infusion therapy education modules improve nursing student knowledge and self-confidence? Methodology: Quasi-experimental pretest-posttest study with 42 nursing students. Analysis:Comparison of pre and post knowledge scores and self-confidence survey results. Results: Statistically significant improvements in post-test knowledge scores (p < 0.001). Conclusions: Knowledge and self-confidence are critical elements for safe infusion therapy practice. Implications for Future Research: Future studies should examine long-term retention of knowledge gains beyond initial training. Implications for Future Practice: Interactive education modules should be integrated into all infusion therapy training programs. |
Tegegne, B., Checkole, D., Shumye, M., Zeru, M., Yalew, Z., Ademe, S., Shiferaw, M., & Edmealem, A. (2025). Knowledge, practice, and factors affecting peripheral intravenous catheters among nurses. BMC Nursing, 24(1). https://doi.org/10.1186/s12912-025-03484-0 | Intervention; Assessment | Research Question: What factors influence nurse knowledge and practice adherence regarding peripheral IV catheters? Methodology: Cross-sectional study of nurses in public hospitals. Analysis: Evaluation of knowledge scores vs. actual clinical PIVC practice. Results: Poor knowledge of aseptic technique was directly linked to higher complication rates. Conclusions: Ongoing structured training is essential to maintain PIVC safety standards. Implications for Future Research: Future research should evaluate training interventions in low-resource hospital settings. Implications for Future Practice: Reinforces need for structured aseptic technique and site assessment training in all settings. |
Feng, T., Hu, L., Yang, Y., Du, C., & Li, J. (2025). Effective strategies for cultivating rapid response, team collaboration, and stress resistance in emergency standardized training nurses. Frontiers in Medicine, 12, 1–7. https://doi.org/10.3389/fmed.2025.1683359 | Intervention; Training | Research Question: How does standardized training cultivate rapid response and team collaboration in nurses? Methodology: Standardized training model evaluation across emergency nursing scenarios. Analysis: Assessment of nurse performance during real rescue and stress scenarios. Results:Standardized training significantly improved stress resistance and clinical efficiency. Conclusions: Structured programs are superior to informal learning for clinical nursing performance. Implications for Future Research: Future research should examine standardized training impact across multiple nursing specialties. Implications for Future Practice: Supports structured competency-based training as the core of the project intervention. |
Calderwood, M. S., Anderson, D. J., Bratzler, D. W., Dellinger, E. P., Garcia, H. S., Maragakis, L. L., Nyquist, A. C., Perkins, K. M., Preas, M. A., Saiman, L., Schaffzin, J. K., Schweizer, M., Yokoe, D. S., & Kaye, K. S. (2023). Strategies to prevent surgical site infections in acute-care hospitals: 2022 update. Infection Control & Hospital Epidemiology, 44(5), 695–720. https://doi.org/10.1017/ice.2023.67 | Intervention; Aseptic Technique | Research Question: What are the updated best practices for preventing healthcare-associated infections? Methodology:Expert consensus and systematic review of infection prevention literature. Analysis: Evaluation of skin preparation protocols and aseptic technique standards. Results: High-quality evidence strongly supports strict aseptic technique during all invasive procedures. Conclusions: Standardization of preparation and technique reduces infection risk across healthcare settings. Implications for Future Research:Future research should evaluate aseptic bundle compliance across diverse clinical populations. Implications for Future Practice: Supports the aseptic technique compliance bundle component of the project intervention. |
PDSA Model References
Reference | Tag | Notes |
Pathan, A., Joshi, M., & Lewis, S. (2024). Utilizing the PDSA cycle to achieve optimal bed utilization and improve the efficiency of a chemotherapy day care unit. Health Services Research and Managerial Epidemiology.https://doi.org/10.1177/23333928241253783 | Model; Framework | Research Question: Can the PDSA cycle improve bed utilization in a chemotherapy day care unit? Methodology:Quasi-experimental quality improvement study using PDSA with lean thinking. Analysis: Process flow mapping and root cause analysis across PDSA phases. Results: Bed utilization increased from 60% to 75% following structured PDSA implementation. Conclusions: The PDSA cycle offered optimal structure for the efficiency improvement initiative. Implications for Future Research: Future studies should test PDSA with lean thinking in other ambulatory clinical units. Implications for Future Practice: PDSA should be used to structure quality improvement initiatives in ambulatory care settings. |
Elhihi, E., Lafi, K., Alahmadi, M., Al-theiba, M., Abdul Rahman, A., Maghrabi, N., Mizi, S., Alsulami, H., Altambkti, M., & Rumbo, T. (2025). Integrating evidence-based practice with PDSA methodology for the reduction of central line associated blood stream infection in intensive care unit. Worldviews on Evidence-Based Nursing.https://doi.org/10.1111/wvn.70096 | Model; Framework; Outcomes | Research Question: Can PDSA integrated with evidence-based practice reduce CLABSI rates in the ICU? Methodology: Evidence-based practice quality improvement project in a 35-bed general ICU. Analysis: Multimodal intervention implementation and evaluation using PDSA methodology. Results: CLABSI rates decreased from 1.37 to 0.62 per 1000 central line days with cost savings of $244,201. Conclusions: PDSA with EBP integration enhances effectiveness, sustainability, and quality of improvement initiatives. Implications for Future Research: Future projects should evaluate PDSA integration with EBP in diverse ICU populations. Implications for Future Practice: PDSA methodology should be routinely integrated with evidence-based practice models for all QI projects. |
Abuzied, Y., Alshammary, S. A., Alhalahlah, T., & Somduth, S. (2023). Using FOCUS-PDSA quality improvement methodology model in healthcare: Process and outcomes. Global Journal on Quality and Safety in Healthcare, 6, 70–72. https://doi.org/10.36401/JQSH-22-19 | Model; Framework | Research Question: How is FOCUS-PDSA applied for quality improvement and enhancement processes in healthcare? Methodology: Descriptive methodology review with two applied clinical quality improvement case examples. Analysis: Review of FOCUS-PDSA application processes and outcomes across two published QI projects. Results: FOCUS-PDSA reduced length of stay and improved palliative care bed capacity in examples. Conclusions: FOCUS-PDSA saves time, money, and effort and supports continuous healthcare quality improvement. Implications for Future Research:Future research should compare FOCUS-PDSA with other QI frameworks across varied settings. Implications for Future Practice: PDSA should be applied systematically to all healthcare process improvement and protocol development initiatives. |
Capella Professors To Choose From For NURS-FPX9010 Class
- Buddy Wiltcher.
- Lisa Kreeger.
(FAQs) related to
NURS FPX 9010 Assessment 2
Question 1: Where can learners access a reliable free sample for NURS FPX 9010 Assessment 2?
Answer 1: From the Tutors Academy website, offering free samples and study resources for NURS FPX 9010 Assessment 2.
Do you need a tutor to help with this paper for you within 24 hours
- 0% Plagiarised
- 0% AI
- Distinguish grades guarantee
- 24 hour delivery
← Previous Assessment: NURS FPX 9010 Assessment 1 | Next Assessment: NURS FPX 9010 Assessment 3 →

